Fifteen years after the U.S. government declared antibiotic-resistant infections to be a grave threat to public health, a Reuters investigation recently found that infection-related deaths are going uncounted, hindering the nation’s ability to fight a scourge that exacts a significant human and financial toll.
Even when recorded, tens of thousands of deaths from drug-resistant infections, as well as many more infections that sicken patients but do not kill them, go uncounted because federal and state agencies do a poor job of tracking them. The Centers for Disease Control and Prevention (CDC), the go-to national public health monitor, and state health departments lack the political, legal and financial wherewithal to conduct rigorous surveillance.
In 2019 — the most recent year CDC data is available — there were 36,242,000 admissions to U.S. hospitals. A conservative standard rate for healthcare acquired infections (HAI) that admitted patients will get during their hospital stays is 5 percent. But some hospitals have an HAI rate of 8 percent or higher.
The 5 percent rate means that of 36.2 million hospital admissions, 1.8 million patients get an HAI, and an 8 percent rate means that of 36.2 million admissions, 2.9 million patients get an HAI.
If the mortality rate for 1.8 million patients is just 10 percent, that means 180,000 Americans die of HAIs annually. If the same mortality rate of 10 percent is applied to 2.9 million HAIs, the number of patient deaths climbs to 232,000. This death rate would place deaths due to HAIs third on the CDC’s list of causes of death in the United States behind heart disease and cancer.
My estimated deaths due to HAIs is considerably higher than the 98,000 the CDC reports on its website and is cited by many reputable papers.
I am keenly aware of the dangers that an unsanitary hospital poses to the safety of patients and staff. Well over one-half of HAI deaths result from a drug-resistant bacterial infection contracted while the patients were receiving hospital care, medical records show. Their death certificates omit any mention of the infections.
The healthcare environment is very complex and features the combination of sick patients, busy staff, a high level of patient care activity and the ongoing stream of visitors. Because of this complexity, the risk of an HAI exists even in the best situation.
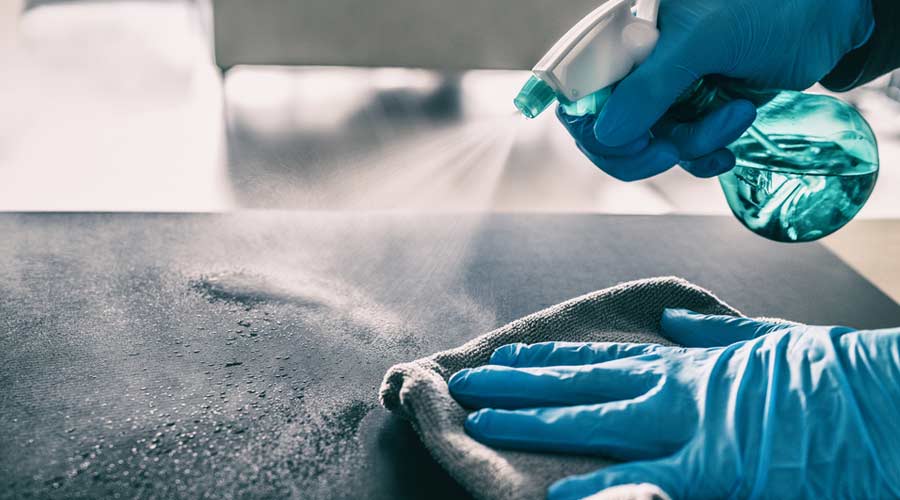
Several studies have demonstrated the persistent contamination of housekeeping surfaces despite the use of traditional cleaning and disinfection methods. This problem has led to widespread acceptance that there is a need to address traditional cleaning processes, as well as to assess the value of secondary disinfectant technologies — kind of the “belt and suspenders” approach to keeping patients and staff safe from contaminated surfaces.
Based on this rethinking of housekeeping, many facilities now look at no-touch disinfection systems, such as ultraviolet-C (UV-C) devices, to augment their manual cleaning processes. These systems have been highly effective against pathogens and spores.
For over 50 years, seatbelts have been installed in cars and trucks to save lives. In 1998, airbags became mandatory in all vehicles made in the United States. It should be noted that the implementation of UV-C technologies is not a substitute for manual cleaning and disinfection but instead is an additional attempt at saving lives. It’s like adding airbags to automobiles to prevent serious injuries.
The use of combined systems — manual cleaning and no-touch disinfection — has been shown to reduce the environmental bioburden, reduce HAIs and address inadequacies and inconsistencies in manual cleaning processes and implementation.
J. Darrel Hicks, BA, MESRE, CHESP, Certificate of Mastery in Infection Prevention, is the past president of the Healthcare Surfaces Institute. Hicks is nationally recognized as a subject matter expert in infection prevention and control as it relates to cleaning. He is the owner and principal of Safe, Clean and Disinfected. His enterprise specializes in B2B consulting, webinar presentations, seminars and facility consulting services related to cleaning and disinfection. He can be reached at darrel@darrelhicks.com, or learn more at www.darrelhicks.com.
 Cleanliness Is a Measurable Outcome
Cleanliness Is a Measurable Outcome Workplace Safety and the Role of Access Control
Workplace Safety and the Role of Access Control Henry Ford Hospital Celebrates Construction Milestone for Expansion Project
Henry Ford Hospital Celebrates Construction Milestone for Expansion Project How EVS Leaders Can Support Staff for Better Cleaning
How EVS Leaders Can Support Staff for Better Cleaning Addressing Infection Prevention Staffing Gaps in Ambulatory and Procedural Care
Addressing Infection Prevention Staffing Gaps in Ambulatory and Procedural Care