The CDC cites healthcare-associated Infections, or HAIs, as the most common adverse hospital-related event, affecting one in 25 patients during their hospital stays. These infections decrease patient safety rates, increase hospital costs and all-too-often result in preventable deaths.
However, recent literature has posited that stopping the spread of HAIs in healthcare settings is as simple as implementing good hand hygiene habits.
Caregivers serve as the most common vehicles of transmission of HAI-causing pathogens – making hand hygiene a crucial component of infection prevention initiatives in the healthcare sphere. Evidence has shown that maintaining stringent hand-hygiene protocol can greatly reduce the rate of HAIs.
Enforcing adherence to proper hand hygiene habits is a challenge in and of itself, due to Healthcare institutions’ reliance on the traditional, yet flawed method to measure compliance – direct observation. The direct observation method consists of an observer being sent to track hand hygiene compliance and provide prompt feedback when improvement is needed.. Unsurprisingly, direct observation yields an inaccurate reading of caregivers’ hand-washing habits, as there is a massive lack of visibility into the rate of behavior actually being confirmed, and is subject to the issue of human error. Additionally, direct observation only offers temporary monitoring, so long-term hand washing behavior is not captured.
Moreover, rates of hand hygiene compliance measured by direct observation can be further skewed by the Hawthorne effect, in which caregivers temporarily change their habits to appear more in-line with protocol, simply because they know they are being watched.
With HAIs at the forefront of adverse event related concerns, and the recent changes made to the Joint Commissions Infection Control Standards, organizations are taking a second look at their hand hygiene compliance monitoring methods – searching for a simpler, more accurate means of stopping the threat of preventable infections.
In a registry style study, individual reporting utilizing CenTrak’s Real-Time Location System (RTLS) badge-based locating technology was put to the test of effectively measuring and improving hand hygiene compliance rates.
Cone Health, Dartmouth Hitchcock Medical Center and Mercy Health Saint Mary’s participated in the 2016 study, where CenTrak’s location-based solutions provided researchers the ability to monitor hand hygiene compliance behavior 100 percent of the time, without the component of human error or Hawthorne effect.
Over the course of the study, CenTrak’s monitoring system collected over 80 months of real-world hand hygiene compliance data from the three healthcare organization participants in a direct bid to examine the impact of technology on hand hygiene compliance rates, and ultimately, aid the collective battle to end the spread of HAIs.
Objectives
Cone Health, Dartmouth Hitchcock Medical Center and Mercy Health Saint Mary’s took part in the 2016 study as a way to compare the discrepancies between their direct observation hand hygiene compliance rates to baseline rates generated by CenTrak’s electronic hand hygiene monitoring system.
The three organizations with electronic monitoring devices at multiple sites set to evaluate the impact of the feedback method utilized by CenTrak’s solutions. The system tracked hand hygiene compliance rates using Group Reporting (in which combined caregiver hand-washing rates are tracked) and Individual Reporting (in which each caregiver’s hand-washing rates are tracked) on caregiver compliance rates.
Methods
CenTrak’s badge-based electronic hand hygiene monitoring system captured caregiver hand hygiene compliance at room entry and exit to form a baseline of caregivers’ actual hand-washing rates. These rates collected with CenTrak’s technology were then compared to the rates that each organization had determined with direct observation prior to implementing the systems. Hand hygiene compliance was measured at the group level and then the individual level to see which method was most effective at reinforcing behavior.
Results
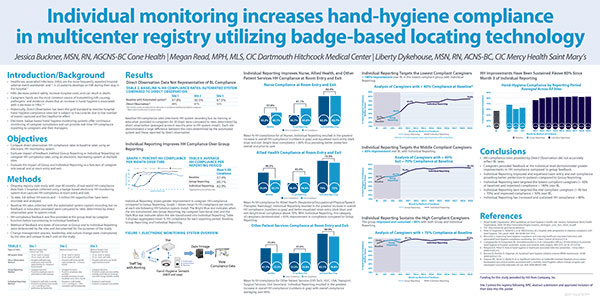
The study shed light on the fact that hand hygiene compliance rates provided by direct observation did not accurately reflect baseline compliance rates. Significant discrepancies between observer-reported and actual caregiver hand washing rates were found within the three institutions.
Cone Health, Dartmouth Hitchcock Medical Center and Mercy Health Saint Mary’s were all pointed to the fact that their baseline hand hygiene compliance rates measured using direct observation were overestimated. With the direct observation method, the three subjects reported an average baseline hand hygiene compliance rate of 89 percent – in other words, 89 percent of caregivers reported that they washed their hands in accordance with their organizations’ protocol.
Data collected by CenTrak’s monitoring system quickly disproved these results, revealing that the three subjects’ average baseline hand hygiene compliance rate, in reality, was approximately 57 percent, meaning that each organization were overestimating their hand hygiene habits.
The study also examined Individual Reporting data and Group Reporting data collected by CenTrak’s monitoring solution, to determine the degree of impact that level of monitoring had on improvement in hand hygiene compliance rates.
Caregivers utilizing CenTrak’s monitoring technology to receive feedback at the individual level demonstrated greater improvements in hand hygiene compliance, raising hand-washing rates across all three hospitals to an average of 83 percent, whereas group feedback yielded an improved baseline rate of only 60 percent in comparison.
The study posited that the implementation of a technology aid in the tracking of hand hygiene compliance was a sustainable solution to improving and maintaining hand hygiene compliance rates. Across three months of individual behavior reporting using CenTrak’s technology, hand hygiene compliance rates were sustained at an average of 80 percent across all three healthcare organizations in the study.

 Laser Scanning: Reducing Risk in Construction Projects
Laser Scanning: Reducing Risk in Construction Projects MOBs Get Smarter and More Complex as Space Pressures Mount
MOBs Get Smarter and More Complex as Space Pressures Mount Ascension Saint Thomas Sets Date for Groundbreaking on New Hospital and Health Campus
Ascension Saint Thomas Sets Date for Groundbreaking on New Hospital and Health Campus Women in Construction Sees Growth on Florida Jobsite
Women in Construction Sees Growth on Florida Jobsite Managing Soft Surfaces, Clean or Soiled
Managing Soft Surfaces, Clean or Soiled